Sun Series: The New Addiction
- Part 1: The painful truth about Nevada (7-6-2008)
- Part 2: Rising use of painkillers taking deadly toll (7-7-2008)
- Part 3: Officials urge action on painkiller abuse (7-8-2008)
Sun Interactive
Audio Clip
- Dr. Mel Pohl, a Las Vegas addiction recovery specialist, discusses the rise of narcotic abuse in the U.S.
-
Audio Clip
- Pohl talks about the nature of addiction.
-
Audio Clip
- Pohl discusses the role that government has played in stopping narcotic abuse.
-
Audio Clip
- Pohl talks about the origins of narcotic abuse.
-
Audio Clip
- Larry Pinson, executive director of the Nevada Pharmacy Board, talks about the rise of narcotics abuse.
-
Audio Clip
- Pinson talks about what the Nevada Pharmacy Board has done to reduce the diversion of prescription drugs.
-
Audio Clip
- Pinson discusses the rise in prescription drug diversion that he has witnessed within the pharmacy field.
-
Audio Clip
- Dr. Michael McKenna, a Las Vegas based pain specialist, discusses the medical movement of pain treatment and its connection with prescribed narcotics.
-
Audio Clip
- McKenna talks about the two sides of opioid medications.
-
Audio Clip
- McKenna discusses the good and bad effects of pain treatment through the use of narcotics.
-
Audio Clip
- McKenna talks about the role of the physician in prescribing narcotics.
-
Beyond the Sun
Reader poll
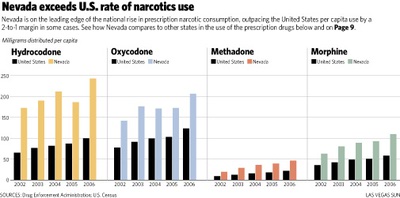
Nevadans consume about twice the national average of several prescription painkillers, making us among the most narcotic-addled populations in the United States, a Sun analysis has found.
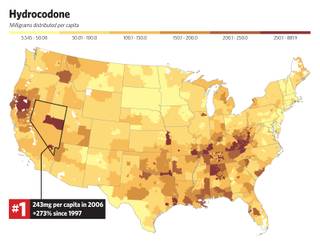
The consequences are deadly. More people in Clark County die of prescription narcotics overdoses than of overdoses of illicit drugs or from vehicle accidents. In 2006, Nevadans were the No. 1 users per capita of hydrocodone — better-known by the brand names Vicodin or Lortab.
We took enough of the drug to equal 48 Vicodin pills for every man, woman and child in the state for a year.
And the numbers are climbing. From 1997 to 2006, the most recent year for which data are available, the per capita rate of hydrocodone used in Nevada jumped by 273 percent.
Nevadans are turning to other narcotic painkillers at an even faster rate.
The per capita use of oxycodone, best-known by the brand name OxyContin, climbed sevenfold from 1997 to 2006, while methadone use jumped 12-fold.
Nevada is ranked fourth in the nation for methadone, morphine and oxycodone use per person, the Sun analysis found.
Following crack cocaine in the 1980s and methamphetamine in the past decade, prescription narcotics are “the next big drug epidemic,” said Matt Alberto, deputy chief of investigations for the Nevada Public Safety Department, the lead prescription drug policing agency in the state.
Emergency room physician Dr. Edwin “Flip” Homansky, medical director of the Valley Health System and a member of the Nevada State Board of Health, said the dramatic rise in prescription narcotic use should be examined.
“When you see increases like that, it’s a warning sign to all of us,” he said, referring to the Sun’s analysis.
The Sun reached its findings after analyzing several thousand pages of Drug Enforcement Administration reports on the state-by-state distribution of controlled substances to pharmacies and health care practitioners. (The DEA monitors the production and distribution of prescription narcotics, which fall into the highest category of regulation for prescription drugs.) After breaking down the data by state populations to reach per capita figures, the Sun determined the highest per person consumption of each prescription narcotic, as well as how consumption has changed over time.
Nevada leads a national trend in the growing use of narcotic painkillers. The National Institute on Drug Abuse reports the number of opiate prescriptions escalated from about 40 million in 1991 to 180 million in 2007 — a 350 percent increase at a time when the nation’s population increased by 19 percent.
A few doctors are doing most of the prescribing. A Sun analysis of a Nevada Pharmacy Board database that tracked all the prescriptions for controlled substances in the state, not just narcotics, showed that in 2007, 1 percent of medical practitioners in the database prescribed 51 percent of controlled substances in the database, and 5 percent of them prescribed 88 percent of the drugs.
No identifying information was made available to the Sun, but experts presume that the heaviest prescribers are pain management and cancer specialists.
Although analyzing individual prescribing habits could hint at who might be overprescribing narcotic painkillers, scrutinizing the database with that intent is banned by statute. Pharmacy board officials said that’s to allow doctors to make judgments and prescribe medicine without fear, which could compromise patient care. The database can be examined by police as part of an active investigation, but authorities can’t use it to go fishing for doctors who can be criminally prosecuted for overprescribing narcotic painkillers.
Assemblywoman Sheila Leslie, D-Reno, said it’s important to understand the factors surrounding the rise in prescription narcotic use and abuse, so legislators may need to “take a closer look” at the law that prevents analyzing the state’s highest prescribers.
Narcotic painkillers are derived from opium, a drug made from poppies that has been used medicinally for thousands of years. Opiate use was common in the United States in the 19th century, and by the early 1900s, when it was recognized that doctors were overprescribing opiates and addiction was a problem, their use was regulated and the drugs fell out of favor. They were mainly prescribed to cancer or terminal patients until the 1990s, when their use was expanded to people with chronic pain. Now we’re in a prescription narcotics boom.
The increasing use of prescription narcotic painkillers in America illustrates the evolving understanding and treatment of pain.
Among the chief challenges to doctors who prescribe potentially addictive painkillers is that pain can be described only subjectively, by the patient. It can’t be measured clinically, like blood pressure or pulse rate.
As a result, pain treatment is both an art and a science. Is the doctor to believe the patient is in pain, or is the doctor being conned by an addict or a drug dealer on the hunt for painkillers? Even the best pain management specialist will say he can’t always tell the difference.
The lines separating prescription narcotic dependence, abuse and addiction are blurry, making it difficult to say whether the skyrocketing drug use is a welcome relief, an epidemic, or something in between.
And experts disagree on how to interpret the growing use of narcotic painkillers. Law enforcement complains about the illegal activity, addiction specialists decry that more people are becoming hooked on drugs, and pain management specialists talk about the benefits of narcotics.
Research on narcotics’ effectiveness in treating pain is inconclusive. In fact, there’s some evidence they can increase pain.
Alarmed experts from all fields agree the rising rate of prescription narcotic use shows no sign of abating.
•••
The use of narcotics to treat pain got a tremendous boost in 1995 from the American Pain Society. Its corporate members include the pharmaceutical companies Purdue, maker of OxyContin; Abbott, maker of Vicodin and UCB, and Watson, maker of the hydrocodone drugs Lortab and Norco.
The society set guidelines saying proper pain management includes urging patients to report unrelieved pain. At the time studies had shown that cancer patients were suffering needlessly because they were not being given enough painkillers.
In January 1999, the Veterans Affairs Department, citing the American Pain Society’s statement that pain is one of the main reasons people consult a doctor, launched a campaign known as “Pain is the Fifth Vital Sign.”
The initiative encouraged health care providers to monitor a patient’s reported level of pain — a subjective symptom — as they did the four measurable vital signs: blood pressure, breathing rate, pulse and temperature. Health care providers asked patients to rank pain on a scale of 1 to 10, and were then urged to treat it.
Dr. Mel Pohl, a Las Vegas addiction recovery specialist, criticizes the pharmaceutical industry’s role in making pain the fifth vital sign.
“The rationale was that we don’t want people to suffer,” Pohl said. “In the best case that’s what it was about. In the worst case, somebody was working this out with the (financial) bottom line in mind. Probably both factors are part of it.”
Soon after, the methods advocated by Veterans Affairs were endorsed by the Joint Commission, the agency that monitors and regulates hospitals. Every hospital is now expected to measure pain in a similar manner.
Dr. Jim Marx, a Las Vegas addiction medicine and pain management specialist, praised the advances, saying doctors now realize they can safely treat patients for pain. This allows patients such as blue-collar workers in Las Vegas to continue in their jobs, he said.
The advent of direct-to-consumer marketing by pharmaceutical companies has also contributed to the rise of prescription narcotics. In 1997, the Food and Drug Administration allowed drug companies to hype their brand-name medicines directly to consumers, which has helped remove any stigma attached to their use. Doctors say patients are now demanding drugs by name.
Homansky, the emergency room doctor, recalled the case of a tourist who said she’d left her bottle of hydrocodone pills at home and needed more. After Homansky recommended a nonnarcotic treatment, she stormed out of the hospital, cursing the staff along the way.
“We’ve had people who get physically abusive, verbally abusive and expect that we’re just there to provide them whatever they want,” Homansky said.
The pharmaceutical companies also market their narcotic painkillers by unleashing cadres of sales representatives on doctors and hosting dinners where physicians offer testimonials about the companies’ medicines.
“There’s a lot of money in the drug industry and they push really hard,” one pain doctor said.
No one can say with certainty why so many narcotic painkillers are used in Nevada, but experts make several educated guesses. The lifestyle of night life and partying leads to more drug-seeking and abuse, doctors said. Also, pain is a complicated symptom of multiple diseases that’s intensified by psychological distress. Las Vegas is a transient place where many people are without social and family support and where the nation’s highest rate of suicide shows a population with mental health problems, doctors said.
The city’s physician shortage also likely plays a role, several experts said. Doctors stressed for time may treat the symptomatic pain rather than explore the problem that’s causing the pain. And once the treatment begins it may continue under the logic that it’s what the patient is accustomed to.
Doctors may further be predisposed to cave in to patients’ requests for narcotics because of how they are reimbursed by insurance companies: by the number of patients they see, not the time spent with each. This may lead providers to take the path of least resistance by writing a prescription. Pohl, the addiction recovery specialist, said it takes doctors “five minutes to say yes and 45 minutes to say no” to a patient’s demand for drugs.
•••
Larry Pinson was browsing in a shop recently when a greeting card caught his eye: “The best part of getting sick is Vicodin,” the card read. “So make sure you save me some, and don’t tell your doctor!”
When greeting cards joke about illegal narcotic abuse, Pinson said, “We’ve got a problem.”
The United States makes up less than 5 percent of the world’s population, but is supplied 99 percent of its hydrocodone and 71 percent of its oxycodone, according to the National Institute on Drug Abuse.
As executive director of the Nevada Pharmacy Board, Pinson presides over the licensing of thousands of pharmacists, pharmacies, technicians and wholesalers, plus about 7,000 doctors, nurse practitioners and dentists who prescribe the drugs and about 180 drug distributors.
About a decade ago the board became aware of the emerging practice of “doctor shopping,” the illegal practice of conniving patients’ visiting multiple providers to get drugs, either to feed an addiction or to sell.
So the Nevada Pharmacy Board created a database that would list every prescription written in the state for certain controlled substances, with the name of the provider and the patient, and the date of the transaction. The monitoring program would help catch patients who might be “doctor shopping.” Regulators from about three dozen other states have followed Nevada’s lead.
A growing number of health care practitioners are using the online database to track their patients’ use of prescriptions. In 1997, the first year of its existence, the database was used 480 times. The number grew exponentially to 65,372 reports in 2007, nearly double from the previous year.
The database flags patients who make a certain number of visits to doctors within an allotted time frame, though officials will not say exactly what type of patient behavior triggers the system, for fear addicts will adjust their behavior accordingly. The database then alerts the doctors to patients who may be shopping for drugs.
Pain management specialists in Las Vegas say the prescription monitoring program is one of many safeguards they use to ensure patients are not abusing painkillers.
“Our attitude is that when a patient leaves our office with a month’s worth of medication, it’s the equivalent of leaving the office with a loaded gun,” said Dr. Michael McKenna, a Harvard- and Stanford-trained pain specialist in Las Vegas.
Among the precautions pain specialists can take to guard against abuse are requiring contracts with patients that discourage doctor shopping, urine tests to verify drug use and monthly visits to track prescriptions and lessen the number of pills a patient has at a given time.
But not every provider takes these precautions.
Jennifer Hilton says that after she had a tooth filled, her dentist handed her a prescription for Vicodin even though she was not complaining about pain. She bristled at the unsolicited prescription because she’s a program coordinator for an inpatient drug addiction program for adolescent girls that’s run by Westcare, a Las Vegas nonprofit that specializes in substance abuse treatment.
Hilton admonished her dentist to ask whether his patients have addiction problems before handing them Vicodin prescriptions.
She said the dentist replied that patients should inform him if they have a drug problem.
“I’m sure some of my clients would have loved to have him as a dentist,” Hilton said, incredulous.
Las Vegas medical professionals repeatedly fail to take addiction seriously, Hilton said. On every clinic visit her teenage drug addicts hand doctors a medical feedback sheet that says: “This person is in a residential treatment facility. Please do not prescribe them anything of a narcotic or addictive nature.”
Still, about one in three kids returns with a narcotic painkiller prescription.
Las Vegas doctors say they are aware of physicians who prescribe whatever drug patients desire, so they will return. It’s good for business.
One drug addict told the Sun addicts share information about the doctors who are quick to write prescriptions.
“If you want (the drugs), you know where to go,” the woman said.
She said a few doctors ran her name through the Nevada Pharmacy Board’s database, recognized her as a doctor shopper and refused to give her drugs. But they never helped her or talked to her about treatment options, she said. Instead they sent her on her way.
The woman, who did not want to be identified, said she is trying to quit drugs and is detoxifying at home. Her only hope is her own motivation to get clean. Her only support is from fellow addicts in her 12-step program.
“I could go to the doctor tomorrow and mess it all up,” she said.
Dr. Jerry Jones, a Las Vegas obstetrician-gynecologist who is president of the Clark County Medical Society, said there may be a few unethical doctors who are overprescribing narcotics. “Most primary care doctors are extremely cautious and conservative about their narcotics prescriptions,” Jones said.
•••
Experts struggle to explain the notably high use of narcotic painkillers in Nevada. Two popular explanations are based on myths or outdated assumptions propagated in the medical community.
Every medical professional interviewed by the Sun cited what each said was Nevada’s aging population — assuming older people need more drugs because they suffer from more cancer or painful chronic conditions.
But U.S. Census figures show that Nevada is actually the 11th-youngest state in the country.
National experts said the same thing, and indeed the median U.S. age — reflecting aging Baby Boomers — rose from 35 in 1997 to 37 in 2007, according to Census figures. But the population aged 65 and older decreased in the same time frame from 12.6 percent to 12.4 percent.
The other common explanation for the high rate of narcotic use was that pain is undertreated in the United States and that Nevada doctors are prescribing more, as they should. But data suggesting the undertreatment of pain are dated and don’t reflect the exponential growth of prescription narcotic use in the past decade.
James Zacny, a psychopharmacologist at the University of Chicago who studies opiates, said the undertreatment of pain is no longer a concern for most patient populations. “I’ve heard the pendulum has swung the other way,” he said. “Now there’s some concern about overprescribing.”
The tragic irony is that painkillers may not work as well as people think. Many doctors say they’re not ideal for long-term use for chronic pain. And some studies show, paradoxically, that they can increase pain. McKenna said the research is relatively new, but shows that some patients actually improve when the medication is withdrawn.
“Pain is very complicated,” McKenna said. “But throwing opiates alone at pain is probably not the best approach.”
On Monday: Skyrocketing use leads to abuse, addiction and death.


Join the Discussion:
Check this out for a full explanation of our conversion to the LiveFyre commenting system and instructions on how to sign up for an account.
Full comments policy